
Treatment-Resistant Depression: When Antidepressants Don't Work — and What to Do Next
You've tried the medications. You've done the work. And still the depression persists. Here's what that means, and what options exist today.
You were told it would work. Maybe it helped a little at first, or maybe it did nothing at all. You adjusted the dose. You switched medications. You tried a second one, then a third. And yet the weight of depression has not lifted — or not lifted enough to let you live the life you want.
If this sounds familiar, you may be experiencing what clinicians call treatment-resistant depression (TRD). It is not a failure of character or effort. It is a clinical reality affecting an estimated 30% of people with major depressive disorder — and it is one of the most actively researched areas in all of psychiatry right now.
The good news is significant: the treatment landscape for TRD has been transformed over the past decade. Options that didn't exist five years ago are now FDA-approved, insurance-covered, and being used successfully by people who had exhausted every prior option. This guide explains what TRD is, how it's defined, why it happens, and — most importantly — what comes next.
What Is Treatment-Resistant Depression?
The most widely used clinical definition of treatment-resistant depression is the failure to achieve adequate response after at least two different antidepressant treatments, each given at an adequate dose for an adequate duration (generally at least four to six weeks). By this standard, research suggests roughly 30–31% of adults with major depressive disorder meet TRD criteria.
It is important to note what TRD is not: it is not the same as depression that was treated incorrectly — with too low a dose, too short a duration, or the wrong medication class. Genuine TRD is diagnosed only after adequate trials have been confirmed. This distinction matters, because many people who believe they have TRD have simply never received an optimized treatment regimen.
TRD is associated with significantly higher healthcare costs, lower quality of life, increased disability, and a substantially greater risk of hospitalization and suicidal ideation compared to depression that responds to first-line treatment.
The Spectrum of Resistance
Depression resistance exists on a spectrum, not as an all-or-nothing state. Some clinicians distinguish between partial non-response (some improvement but not remission), full non-response (no meaningful change), and chronic treatment resistance (long-term failure across multiple treatment modalities). Understanding where on this spectrum a patient falls shapes which interventions are most appropriate.
Why Do Some People Not Respond to Antidepressants?
No single factor causes treatment resistance. In many cases, it is the result of several overlapping mechanisms working together:
- Biological heterogeneity: Depression is not one disease — it is many conditions that share similar surface symptoms. A person whose depression is driven primarily by inflammatory processes may not respond to serotonin-targeting medications at all, because their underlying biology is different.
- Pharmacogenomic differences: Genetic variations affect how individuals metabolize psychiatric medications. Some people are "ultra-rapid metabolizers" of certain antidepressants, meaning the drug is cleared from their system before it can take effect. Pharmacogenomic testing — matching medications to your genetic profile — can help identify this.
- Undiagnosed co-occurring conditions: Untreated anxiety disorders, sleep disorders, sleep apnea, thyroid dysfunction, autoimmune conditions, or unrecognized bipolar disorder all dramatically reduce the effectiveness of antidepressant treatment.
- ADHD overlap: Untreated ADHD can masquerade as or worsen depression. Many adults with TRD have undiagnosed ADHD driving persistent dysphoria.
- Neurobiological factors: Chronic depression causes measurable changes in brain structure, including shrinkage of the hippocampus and disruption of prefrontal-limbic circuits. Standard antidepressants do not fully reverse these changes, but some newer treatments may.
- Trauma and psychosocial stressors: Ongoing adverse circumstances — unstable housing, trauma exposure, abusive relationships, poverty — act as constant biological stressors that blunt medication response.
Could This Be Treatment-Resistant Depression?
Check any statements that are true for your experience. This is not a clinical tool, but it may help you recognize whether a more comprehensive evaluation is warranted.
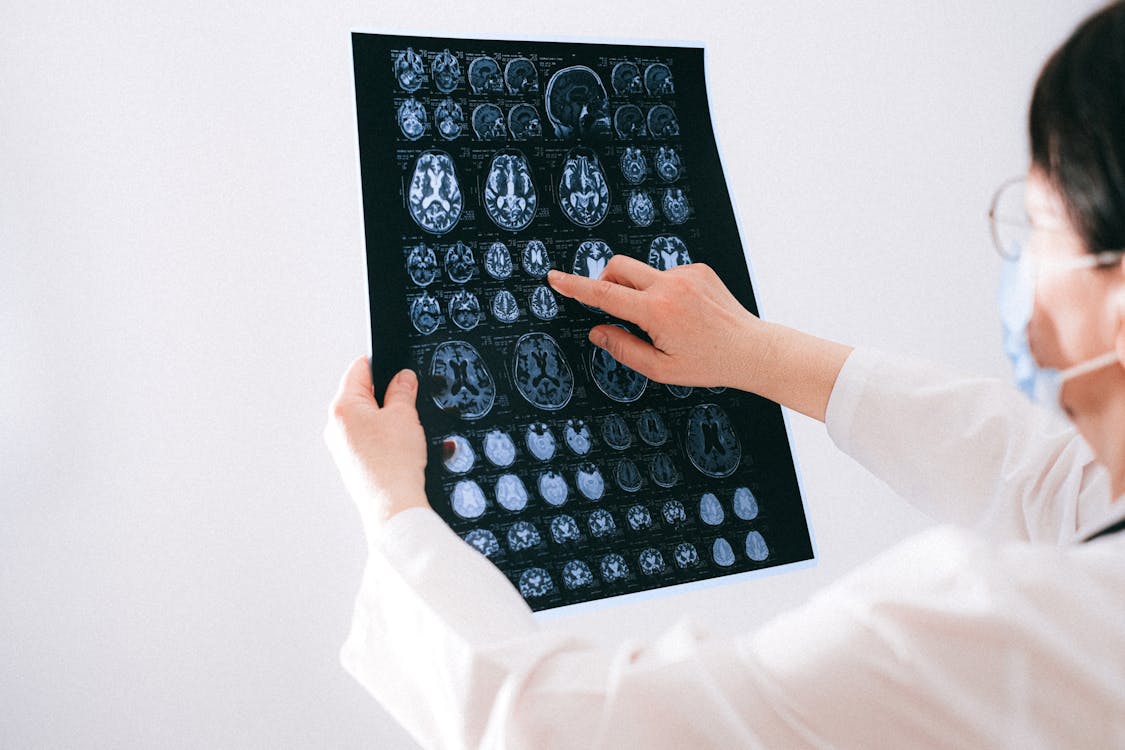
Comprehensive evaluation — including assessment for co-occurring conditions, pharmacogenomic testing, and a full treatment history review — is often the most important first step when standard antidepressants haven't worked.
Before Assuming TRD: What a Comprehensive Evaluation Covers
Many people diagnosed with treatment-resistant depression have actually experienced inadequate treatment — not true biological resistance. Before pursuing advanced interventions, a thorough reassessment should cover:
- Were prior medications dosed adequately and taken for sufficient duration?
- Were adherence issues or absorption problems (e.g., due to GI conditions) a factor?
- Has a diagnosis of bipolar disorder been ruled out? Antidepressants alone are inappropriate — and potentially destabilizing — for bipolar depression.
- Have co-occurring sleep disorders, anxiety disorders, ADHD, thyroid problems, or autoimmune conditions been evaluated and addressed?
- Has evidence-based psychotherapy (particularly CBT or behavioral activation) been adequately trialed alongside medication?
A specialist evaluation — such as those conducted by East Coast Telepsychiatry's board-certified psychiatrists via secure telehealth video — can answer these questions systematically and identify paths forward that may have been missed.
Today's Most Effective Treatments for TRD
This is where the landscape has genuinely changed. The past decade has produced more validated, accessible treatment options for TRD than any period before it. The right choice depends on severity, urgency, treatment history, and individual medical factors — but the options below now represent a robust toolkit for patients whose depression has resisted standard care.
Medication Strategies: Optimization & Augmentation
Before escalating to more intensive interventions, evidence-based medication optimization should be completed. This includes augmentation — adding a second agent to an existing antidepressant to boost response. Well-studied augmentation options include lithium, atypical antipsychotics (aripiprazole, quetiapine, olanzapine), thyroid hormone, and buspirone. Combination antidepressant strategies (e.g., SSRI + bupropion, or SSRI + mirtazapine) are also commonly used.
Esketamine (Spravato): The FDA-Approved Breakthrough
In 2019, the FDA approved esketamine (brand name Spravato) as a nasal spray specifically for treatment-resistant depression — the first entirely new pharmacological mechanism approved for depression in over three decades. Unlike standard antidepressants, which work by increasing serotonin, norepinephrine, or dopamine, esketamine targets the glutamate system — the brain's most abundant neurotransmitter — triggering rapid neuroplasticity and synaptic repair.
Key facts about esketamine:
- Works within hours to days rather than weeks — especially significant for people experiencing severe impairment or suicidal ideation
- Must be self-administered under clinical supervision, with a mandatory 2-hour monitoring period after each dose
- Must be combined with an oral antidepressant
- Often covered by insurance with prior authorization for qualifying TRD diagnoses
- Phase 3 clinical trial (SUSTAIN-1) demonstrated a 51% reduction in relapse risk for stable remitters who continued treatment
- Is the only FDA-approved agent (alongside lithium) proven to reduce suicidal ideation acutely
"Esketamine is different than any other antidepressant in that it not only prevents the neurotoxic effects of depression on the brain, but it also seems to have a growth-promoting effect."
— Adam Kaplin, MD, PhD, Johns Hopkins MedicineIV Ketamine
Intravenous (IV) ketamine — the racemic form of the drug — has been used off-label for TRD since the early 2000s and remains one of the fastest-acting treatments available. Meta-analyses of over 24 randomized controlled trials show response and remission rates that significantly exceed those of most antidepressants. A single infusion produces a 50–70% response rate in patients who have failed multiple other treatments. IV ketamine offers greater dose precision than the nasal spray formulation, but because it is off-label for depression, it is not typically covered by insurance.
Transcranial Magnetic Stimulation (TMS)
TMS is a completely medication-free, FDA-cleared procedure that uses focused magnetic pulses to stimulate underactive brain circuits in the prefrontal cortex — a region directly implicated in depression. It is non-invasive, requires no anesthesia, and is performed while the patient remains fully awake. Standard TMS protocols run 4–6 weeks of daily sessions. A newer protocol — the SAINT protocol (accelerated theta-burst stimulation), FDA-cleared in 2022 — compresses treatment into five consecutive days and has demonstrated remission rates approaching 80% in some trials. Medicare began covering SAINT at a defined reimbursement rate in July 2025.
Electroconvulsive Therapy (ECT)
Despite its outdated reputation, modern ECT is a highly effective, evidence-based treatment and remains one of the most potent interventions for severe, life-threatening depression. Conducted under brief general anesthesia, ECT produces response rates of 60–80% in TRD — higher than any other single treatment modality. Memory side effects, which were more pronounced with older techniques, have been substantially reduced with modern brief-pulse and ultrabrief-pulse protocols.
Psychedelic-Assisted Therapy: On the Horizon
Psilocybin-assisted therapy for TRD is the most closely watched emerging treatment in psychiatry. In early 2026, COMPASS Pathways reported positive Phase 3 trial results for COMP360, a synthetic psilocybin compound for treatment-resistant depression — potentially placing the first psilocybin-based medication within reach of FDA submission. Broad clinical availability is likely 1–2 years away pending regulatory review. For patients who cannot wait, clinical trial enrollment remains an option in many states.
Esketamine (Spravato)
Nasal spray for TRD. Rapid onset (hours), targets glutamate/NMDA. Insurance-covered with prior auth. Requires in-clinic administration.
IV Ketamine
Fastest-acting option (50–70% response). Off-label, generally self-pay. Ideal for severe or urgent TRD. Multiple infusions over 3–6 weeks.
TMS / SAINT Protocol
Non-invasive, medication-free. Standard: 6 weeks daily. SAINT: 5 days intensive with ~80% remission in trials. Medicare-covered from mid-2025.
Electroconvulsive Therapy
60–80% response rate. Modern ECT is safe and targeted. Best for severe, life-threatening, or psychotic depression. Often covered by insurance.
Medication Augmentation
Adding lithium, atypical antipsychotics, or thyroid hormone to existing antidepressants. First escalation step for many patients.
Psilocybin Therapy
Positive Phase 3 results in 2026. FDA submission anticipated. Currently available via clinical trials. Transformative but not yet broadly accessible.

Recovery from treatment-resistant depression is not only possible — it is being achieved every day by patients who found the right combination of treatments after standard antidepressants failed them.
What to Do If You Think You Have TRD
In the meantime, here are concrete steps you can take right now:
- Document your full medication history — every antidepressant you've tried, the dose, duration, and what happened. Your psychiatrist will need this to evaluate whether your prior trials were truly adequate.
- Rule out contributing medical conditions. Ask your primary care provider to check your thyroid, inflammatory markers, vitamin D, and B12 levels. Sleep apnea in particular is dramatically underdiagnosed and directly worsens depression.
- Address sleep. Chronic sleep disruption is both a symptom and a driver of treatment-resistant depression. A comprehensive sleep evaluation should be part of any TRD workup.
- Ask about pharmacogenomic testing. A simple cheek swab can identify how your body metabolizes different medications — reducing the guesswork in prescribing.
- Don't give up on therapy. Cognitive behavioral therapy specifically adapted for treatment-resistant depression (including behavioral activation and metacognitive therapy) produces meaningful results when medications alone haven't — and is most powerful in combination with pharmacological treatment.
- Ask directly about esketamine, TMS, and ketamine. These are no longer experimental — they are first-line options for TRD and your psychiatrist should be prepared to discuss whether you're a candidate.
You Haven't Run Out of Options — You Need a Specialist
If standard antidepressants haven't worked, a comprehensive evaluation with a board-certified psychiatrist may reveal paths forward you haven't tried yet. We offer secure, same-week telehealth appointments across the East Coast.
Book Your EvaluationMost major insurance plans accepted | Same-week appointments available | If you're in crisis, call or text 988
Sources & Further Reading
- Zhdanava M, et al. The Prevalence and National Burden of Treatment-Resistant Depression. J Clin Psychiatry. 2021. psychiatrist.com
- Fiorillo A, et al. Treatment Resistant Depression: Epidemiology, Clinic, Burden and Treatment. Front. Psychiatry. 2025. frontiersin.org
- Johns Hopkins Medicine. Esketamine for Treatment-Resistant Depression. hopkinsmedicine.org
- Cognitive FX. Treatment-Resistant Depression: Guide to Evidence-Based Treatments 2026. cognitivefxusa.com
- PMC. Innovative Approaches in Treatment-Resistant Depression. Front. Psychiatry. 2024. pmc.ncbi.nlm.nih.gov
- COMPASS Pathways. Phase 3 COMP360 Psilocybin Trial Results. 2026.
- SPRAVATO® (esketamine) Prescribing Information. Janssen Pharmaceuticals. spravato.com
- National Depression Hotline. Depression Treatment Statistics 2026. nationaldepressionhotline.org
